Why Understanding Cost‑Sharing Matters for Parents
Pediatric health costs can quickly add up, especially for families managing chronic conditions or frequent specialist visits. Understanding the core insurance concepts—copayments, deductibles, coinsurance, and out‑of‑pocket maximums—helps parents anticipate what they will owe at each appointment and avoid surprise bills. Preventive services such as well‑child exams and immunizations are often covered with no cost‑sharing, reducing overall spending and catching health issues early. By knowing how these cost‑sharing elements work, families can budget wisely, choose plans that match their child’s needs, and keep essential care affordable each year for lasting health.
Navigating Washington’s Child Health Coverage Options
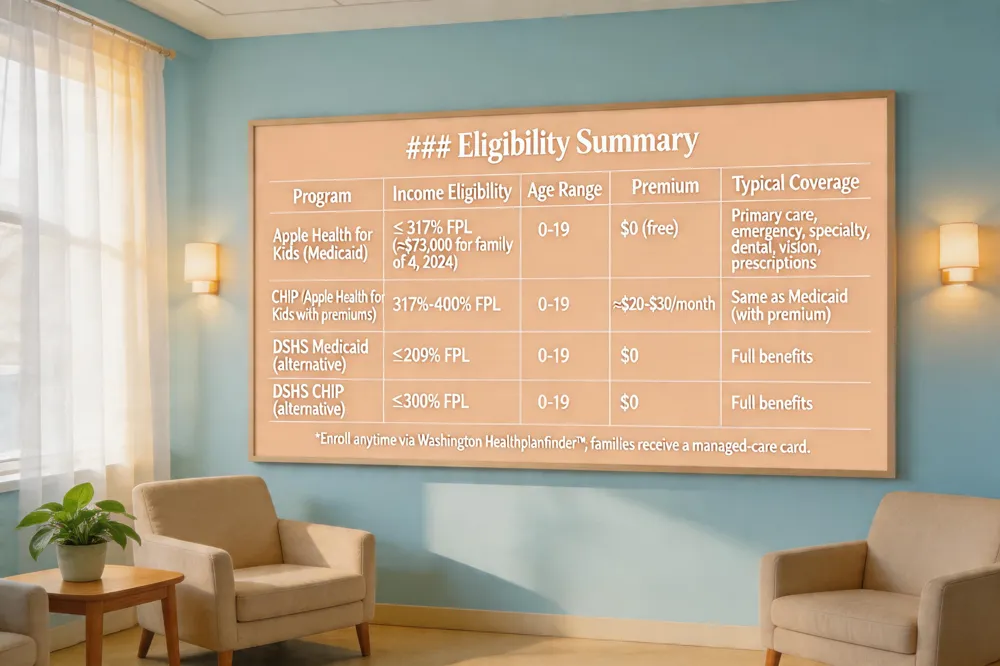
Eligibility Summary
| Program | Income Eligibility | Age Range | Premium | Typical Coverage |
|---|---|---|---|---|
| Apple Health for Kids (Medicaid) | ≤ 317 % FPL (≈ $73,000 for a family of 4 in 2024) | 0‑19 | $0 (free) | Primary care, emergency, specialty, dental, vision, prescriptions |
| CHIP (Apple Health for Kids with premiums) | 317 %‑400 % FPL | 0‑19 | Modest monthly premium (≈ $20‑$30) | Same as Medicaid, but with premium |
| DSHS Medicaid (alternative) | ≤ 209 % FPL | 0‑19 | $0 | Full benefits |
| DSHS CHIP (alternative) | ≤ 300 % FPL | 0‑19 | $0 | Full benefits |
Enroll anytime via Washington Healthplanfinder™; families receive a managed‑care card.
 Washington provides free or low‑cost health insurance for children through Apple Health for Kids (Medicaid) and the Children’s Health Insurance Program (CHIP).
Washington provides free or low‑cost health insurance for children through Apple Health for Kids (Medicaid) and the Children’s Health Insurance Program (CHIP).
Free health insurance for children in Washington state – Families with household income up to 317 % of the Federal Poverty Level (FPL) qualify for Apple Health for Kids, while CHIP serves those with slightly higher incomes. Enroll anytime via Washington Healthplanfinder™; approved families receive a managed‑care card and coverage for primary care, emergency visits, specialty care, dental, vision, and prescriptions.
Washington Apple Health (Medicaid) for children – eligibility and income limits – Children age 0‑19 whose family income is at or below 317 % FPL (≈ $73,000 for a family of four in 2024) are eligible. Residency and citizenship/immigration status are required. Premium‑based Apple Health for Kids is available for incomes above the Medicaid threshold but below state limits. Income is verified through Modified Adjusted Gross Income and updated online.
Children’s Health Insurance Program (CHIP) in Washington – eligibility – CHIP (also called Apple Health for Kids with premiums) covers children under 19 whose income falls between 317 % and 400 % FPL. A modest monthly premium may apply.
DSHS health insurance eligibility for children in Washington – The Department of Social and Health Services determines eligibility by income (up to 209 % FPL for Medicaid, up to 300 % FPL for CHIP), residency, and citizenship/immigration status. Applications are processed year‑round via WashingtonConnection.org.
Cost‑Sharing Basics: Deductibles, Copays, and Coinsurance
Cost‑Sharing Pillars
| Pillar | Definition | When it Applies | Example |
|---|---|---|---|
| Deductible | Amount you must pay out‑of‑pocket before insurer shares costs | Begins at start of plan year, resets annually | $500 deductible for a HDHP |
| Copay | Fixed fee per service | May apply before or after deductible depending on plan | $30 for a well‑child visit |
| Coinsurance | Percentage of allowed charge after deductible | Applied after deductible is met | 20 % of a $200 specialist visit = $40 |
| Out‑of‑Pocket Maximum | Cap on total OOP spending (deductible + copays + coinsurance) | Once reached, insurer pays 100 % for rest of year | $3,000 maximum |
All amounts count toward the out‑of‑pocket maximum.
 Understanding the three pillars of health‑plan cost‑sharing—deductible, copay, and Coinsurance—helps families budget pediatric care with confidence. A deductible is the total amount you must spend out‑of‑pocket each plan year before the insurer begins to share costs; it resets annually. A copay is a fixed fee you pay at the time of a specific service (e.g., $30 for a well‑child visit). Some plans charge copays only after the deductible is satisfied, while others apply them regardless. Coinsurance is a percentage of the allowed charge you owe after the deductible is met (e.g., 20%). All copays, coinsurance payments, and any remaining deductible balance count toward your out‑of‑pocket maximum. Once that cap is reached, the insurer pays 100 % of additional covered services for the rest of the year.
Understanding the three pillars of health‑plan cost‑sharing—deductible, copay, and Coinsurance—helps families budget pediatric care with confidence. A deductible is the total amount you must spend out‑of‑pocket each plan year before the insurer begins to share costs; it resets annually. A copay is a fixed fee you pay at the time of a specific service (e.g., $30 for a well‑child visit). Some plans charge copays only after the deductible is satisfied, while others apply them regardless. Coinsurance is a percentage of the allowed charge you owe after the deductible is met (e.g., 20%). All copays, coinsurance payments, and any remaining deductible balance count toward your out‑of‑pocket maximum. Once that cap is reached, the insurer pays 100 % of additional covered services for the rest of the year.
Copay vs deductible – how they work: The deductible is a threshold; the copay is a per‑visit charge that may apply before or after the threshold is met.
What does a $40 copay after deductible mean?: First you pay the full deductible. After that, each qualifying visit costs a fixed $40, which counts toward your out‑of‑pocket maximum but not toward the deductible.
How do copay, deductible, and out‑of‑pocket maximum work together?: Pay the deductible, then copays/coinsurance for each service; all these amounts accumulate toward the out‑of‑pocket maximum, after which the plan covers all further costs.
Typical Out‑of‑Pocket Costs for Pediatric Visits
Typical OOP Costs (In‑Network)
| Service | Copay Range | Coinsurance (if deductible met) | Notes |
|---|---|---|---|
| Routine well‑child visit | $10‑$30 | – | Often $20‑$50 per visit |
| Urgent‑care visit | $35‑$75 | 15‑%30 % after deductible | Higher if deductible already met |
| Emergency‑room visit | $100‑$150 | – (plus tests/procedures) | Initial copay; additional charges may apply |
| Pediatric cardiology specialist | $25‑$60 | 20‑30 % after deductible | Out‑of‑network can be much higher |
| Facility fee (hospital‑based urgent care) | $0‑$50 (if any) | – | May not be covered unless in‑network |
Out‑of‑network care may result in balance billing.
 Parents can expect a modest, fixed copay for routine pediatric appointments—generally $10‑$30, though many plans list $20‑$50 per visit. Urgent‑care visits are somewhat higher, typically $35‑$75, and may shift to a 15%‑30% coinsurance if the family’s deductible has already been met. Emergency‑room visits start at $100‑$150 for the initial copay, with additional charges for tests or procedures. Specialist care, such as pediatric cardiology, often carries a copay of $25‑$60 or a coinsurance of 20%‑30% after the deductible, and the amount can rise sharply if the provider is out‑of‑network. In‑network providers have negotiated rates that keep copays and coinsurance low, while out‑of‑network care may require the full allowed charge or a higher percentage of cost‑sharing, sometimes resulting in balance billing. Understanding these tiers helps families budget for regular check‑ups, urgent needs, and specialty referrals while minimizing unexpected out‑of‑pocket expenses.
Parents can expect a modest, fixed copay for routine pediatric appointments—generally $10‑$30, though many plans list $20‑$50 per visit. Urgent‑care visits are somewhat higher, typically $35‑$75, and may shift to a 15%‑30% coinsurance if the family’s deductible has already been met. Emergency‑room visits start at $100‑$150 for the initial copay, with additional charges for tests or procedures. Specialist care, such as pediatric cardiology, often carries a copay of $25‑$60 or a coinsurance of 20%‑30% after the deductible, and the amount can rise sharply if the provider is out‑of‑network. In‑network providers have negotiated rates that keep copays and coinsurance low, while out‑of‑network care may require the full allowed charge or a higher percentage of cost‑sharing, sometimes resulting in balance billing. Understanding these tiers helps families budget for regular check‑ups, urgent needs, and specialty referrals while minimizing unexpected out‑of‑pocket expenses.
Newborn Coverage and Early Enrollment
Newborn Enrollment Checklist
| Step | Action | Deadline |
|---|---|---|
| 1 | Notify Health Care Authority (online or 1‑800‑562‑3022) | Within 30 days of birth |
| 2 | Verify automatic Apple Health for Kids eligibility (if parent enrolled) | Immediate |
| 3 | If needed, enroll in premium‑based CHIP (≈ $20‑$30/mo) | Within enrollment window |
| 4 | For private plans, use Washington Health Benefit Exchange during open or special enrollment | Within 60 days of birth |
| 5 | Submit newborn’s birth certificate & SSN | At enrollment |
| 6 | Confirm network status & any copay/deductible requirements before first visit | Before first appointment |
Contact AskMAGI@hca.wa.gov for assistance.
 Washington families enjoy streamlined options for newborn health insurance. Automatic eligibility for Apple Health for Kids: If a parent is already enrolled in Apple Health (Medicaid) or meets the state’s income limits, the newborn is automatically eligible for Apple Health for Kids, providing full coverage with no premiums, deductibles, or co‑pays. Premium‑based CHIP enrollment options: Families whose income is slightly above Medicaid thresholds can enroll the infant in Apple Health for Kids with a modest monthly premium ($20–$30), the state’s CHIP equivalent. Steps to add a newborn to private or public plans: 1) Notify the Health Care Authority online or by phone (1‑800‑562‑3022) within 30 days of birth to trigger automatic enrollment. 2) If choosing a private plan, use the Washington Health Benefit Exchange during open enrollment or a special enrollment period after birth, submitting the newborn’s birth certificate and Social Security number. 3) Verify network status and any co‑pay or deductible requirements before the first visit. For assistance, contact AskMAGI@hca.wa.gov.
Washington families enjoy streamlined options for newborn health insurance. Automatic eligibility for Apple Health for Kids: If a parent is already enrolled in Apple Health (Medicaid) or meets the state’s income limits, the newborn is automatically eligible for Apple Health for Kids, providing full coverage with no premiums, deductibles, or co‑pays. Premium‑based CHIP enrollment options: Families whose income is slightly above Medicaid thresholds can enroll the infant in Apple Health for Kids with a modest monthly premium ($20–$30), the state’s CHIP equivalent. Steps to add a newborn to private or public plans: 1) Notify the Health Care Authority online or by phone (1‑800‑562‑3022) within 30 days of birth to trigger automatic enrollment. 2) If choosing a private plan, use the Washington Health Benefit Exchange during open enrollment or a special enrollment period after birth, submitting the newborn’s birth certificate and Social Security number. 3) Verify network status and any co‑pay or deductible requirements before the first visit. For assistance, contact AskMAGI@hca.wa.gov.
Special Considerations for Pediatric Cardiology and Specialty Care
Cardiology Cost Factors
| Factor | In‑Network | Out‑of‑Network |
|---|---|---|
| Provider Rate | Negotiated lower allowed charge | Full provider charge |
| Copay / Coinsurance | Applies to lower allowed amount (e.g., $40 copay) | May be higher percentage or full charge |
| Facility Fee | Often waived or lower | May be added (e.g., $100‑$200) |
| HDHP Deductible | Must be met before any sharing (e.g., $500‑$1,000) | Same, but higher allowed charges increase OOP |
| Financial Tools | HSAs/FSAs can reimburse deductible/coinsurance | Same, but higher outlay needed |
Confirm cardiology clinic is in‑network to reduce OOP costs.
 When you schedule a pediatric cardiology appointment, the biggest factor influencing your out‑of‑pocket (OOP) cost is whether the provider is in‑network providers have negotiated rates. In‑network cardiologists have negotiated rates, so your copay, coinsurance and deductible apply to a lower allowed charge; out‑of‑network doctors often use the full charge, leading to higher coinsurance percentages or even balance billing.
When you schedule a pediatric cardiology appointment, the biggest factor influencing your out‑of‑pocket (OOP) cost is whether the provider is in‑network providers have negotiated rates. In‑network cardiologists have negotiated rates, so your copay, coinsurance and deductible apply to a lower allowed charge; out‑of‑network doctors often use the full charge, leading to higher coinsurance percentages or even balance billing.
Facility fees are another hidden expense. Many urgent‑care centers and hospitals add a separate building‑use charge that insurers may not cover unless the visit occurs in a hospital emergency room. Practices like Little Spurs Pediatric Urgent Care avoid facility fee, keeping OOP costs more predictable for families.
If your family is enrolled in a high‑deductible health plan (HDHP), you must meet the deductible before the insurer shares any cost. Specialist visits, imaging studies, and cardiac procedures typically have higher allowed amounts, so a $500‑$1,000 deductible can translate into substantial OOP payments before coinsurance kicks in. Using HSAs or FSAs can help offset these expenses, and confirming that the cardiology clinic is in‑network before the visit can dramatically reduce the financial burden.
Financial Tools: HSAs, FSAs, and Assistance Programs
Financial Resources Overview
| Tool | Eligibility | Tax Benefits | Typical Use |
|---|---|---|---|
| HSA (Health Savings Account) | Paired with HDHP | Contributions pre‑tax, growth tax‑free, withdrawals tax‑free for qualified medical expenses | Pay deductible, coinsurance, copays |
| FSA (Flexible Spending Account) | Offered by employer | Contributions pre‑tax, use within plan year (or grace period) | Routine pediatric meds, labs, specialist visits |
| Direct Primary Care (e.g., Zest Pediatrics) | Membership fee (≈ $5/day) | Not tax‑advantaged but predictable cost | Unlimited illness visits, in‑office labs, no facility fees |
| Apple Health for Kids / CHIP | Income‑based eligibility | $0‑$10 copays, no deductible for many services | Primary, specialty, dental, vision, prescriptions |
| Community Assistance (Easterseals, UnitedHealthcare Children’s Foundation) | Varies | May provide grants or counseling | Help with OOP, explain benefits, referral services |
Leverage HSAs/FSAs to offset HDHP costs and consider DPC for predictable budgeting.
 Tax‑advantaged accounts such as Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs) let families set aside pre‑tax dollars to pay copays, deductibles, coinsurance, and other out‑of‑pocket (OOP) costs. HSAs are paired with high‑deductible health plans, while FSAs are offered by many employers and can be used for qualified pediatric expenses, including medication, lab tests, and specialist visits.
Tax‑advantaged accounts such as Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs) let families set aside pre‑tax dollars to pay copays, deductibles, coinsurance, and other out‑of‑pocket (OOP) costs. HSAs are paired with high‑deductible health plans, while FSAs are offered by many employers and can be used for qualified pediatric expenses, including medication, lab tests, and specialist visits.
Direct Primary Care (DPC) memberships, like the Zest Pediatrics model in Federal Way, charge a flat daily fee (≈ $5) that covers unlimited illness visits, in‑office labs, and eliminates facility fees, often resulting in lower annual OOP spending compared with traditional fee‑for‑service billing.
Community resources reinforce these tools: Washington’s Apple Health for Kids and CHIP provide $0‑$10 co‑pays and no deductibles for many services; local health‑care alliances and pediatric offices offer financial counseling, assistance with Explanation of Benefits, and referrals to programs such as Easterseals or the UnitedHealthcare Children’s Foundation. Leveraging these options helps families manage pediatric health costs while ensuring uninterrupted care.
Putting It All Together for Your Family’s Health
Each year, carefully review your insurance summary, noting copay amounts, deductibles, and out‑of‑pocket caps. Schedule all covered preventive visits—well‑child exams and immunizations—to avoid cost‑sharing. Combine Health Savings or Flexible Spending Accounts with Washington’s Apple Health for Kids and CHIP to pay qualified expenses tax‑free, minimizing out‑of‑pocket bills for child's health today.
